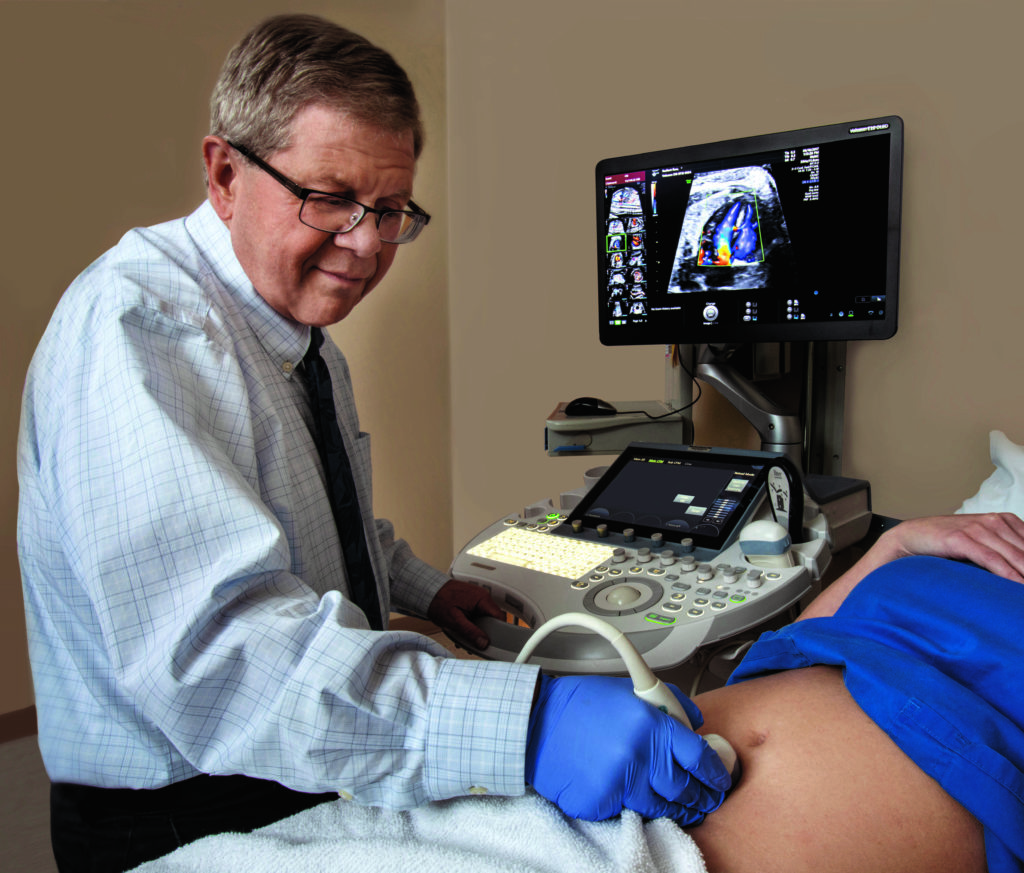

OWENSBORO With forty years in the field of perinatology, Thomas Tabb, MD, has seen extraordinary advancements, both in technology and thinking within the specialty. “Maternal-fetal medicine initially focused on the mother with conditions like hypertension, diabetes, and lupus. Our ultrasound equipment, when things started, was really not mature enough to do a lot more with the fetus. As things have evolved, the maternal part is obviously still important for management of diseases, but now we’ve gone into other areas with respect to the fetus,” says Tabb, who is board certified in both obstetrics/gynecology and maternal-fetal medicine.
After earning his medical degree from the University of Kentucky, Tabb completed his internship, residency, and a maternal-fetal medicine fellowship at the University of Tennessee in Memphis. He also gained a post-doctoral fellowship at McMaster University in Hamilton, Ontario, Canada. Throughout his career, Tabb has passed on his extensive knowledge through teaching at several facilities including the University of Tennessee; McMaster University; the University of Texas Medical Branch in Galveston; and both the University of Kentucky College of Medicine and University of Louisville. Tabb also served as an editorial consultant for Protocol Reviews in Obstetrics & Gynecology, a publication affiliated with John Hopkins University.
In 2016, when the Owensboro Health Medical Group expanded its offerings to include a maternal-fetal medicine department along with its neonatal intensive care unit, Tabb, who was living and practicing in Louisville, saw it as the perfect opportunity to make a change. He says, “I wanted a little different type of practice and I wanted a little different type of town.”
Patient Population Increasing
As a maternal-fetal medicine specialist, Tabb cares for women experiencing complicated or high-risk pregnancies and focuses on managing the mother’s existing health problems throughout the pregnancy and birth and beyond. These most often include diabetes, obesity, substance abuse, chronic hypertension, preexisting maternal cardiovascular disease, and lupus. Of the western Kentucky population, up to 25% of pregnant women require a maternal-fetal specialist, the majority due to obesity and diabetes.
“I think diabetes is the biggest driving force we’re seeing now, as far as having issues with cardiac and pulmonary problems. As the incidence of diabetes increases, the incidence of cardiovascular abnormality in the fetus goes up. We’re seeing that more and more. The incidence of cardiac abnormalities in this area is quite significant,” states Tabb.
A New Generation of Ultrasound
Fortunately, one of the most significant advancements has been in the realm of fetal heart monitoring. According to Tabb, “The ultrasound equipment we initially had did not have the ability to define what was going on in the fetal heart other than just saying there was a heartbeat. The technology has advanced enough now where even very minute structural abnormalities can be detected.”
Today’s fetal echocardiography provides a highly detailed picture of a baby’s heart, revealing early insight into structural anomalies and congenital heart defects.
Of course, it is absolutely essential that high risk patients receive fetal echocardiograms, but the procedure is now advised and accessible to all pregnant women seen by the Maternal Fetal Medicine practice. “The fetal echocardiogram has become a standard for every pregnant patient in our practice. Traditionally people would say the only patients who need fetal echo are women who are at increased risk, for example the diabetic patient or patient who has a history of heart disease in the family, but here we basically do a fetal echo on every patient we do ultrasounds on,” explains Tabb.
In many instances when the fetus has life-threatening abnormalities, the mothers do not have obvious risk factors, including familial heart disease. Tabb says, “You would be surprised at the number of abnormalities we see in mothers who, if you go by the book, have no known risk factors for fetal heart disease.”
Upon delivery, these infants often require immediate attention by a pediatric cardiologist, and in some cases surgery. Therefore, it is crucial the delivery be scheduled at a facility providing cardiac services. Tabb stresses, “You want to make sure they prenatally choose an appropriate place for delivery where pediatric cardiology and pediatric cardiothoracic surgery are available.”
He goes on to say, “The goal for the state should be that every baby with fetal heart disease should be identified and delivered at a tertiary center with pediatric cardial facilities available.”
As for the future, early detection is the goal. Tabb states, “We’re trying to start a program to do fetal echocardiograms in the first trimester and identify the cardiac defects even at twelve to fourteen weeks. Everything is going to be earlier and earlier when it comes to diagnosis.”


